In news that came after the Gist Weekly’s deadline, the U.S. Supreme Court on Friday ruled that the president does not have the authority to use his emergency powers to unilaterally impose tariffs. This appears to threaten many tariffs currently in place, which have impacted many industries including healthcare. The Gist Weekly team is studying the ruling, with more to report as the story develops.
IN THE NEWS
The biggest news of the week—and what we think about it.
- FTC appeals judicial ruling on pre-merger notification. The Federal Trade Commission (FTC) yesterday appealed a Texas judge’s order nullifying its expanded pre-merger reporting rule under the Hart-Scott-Rodino Act. The rule, which was finalized in 2024 and took effect in 2025, requires certain merging organizations to submit significantly more information up front, including expanded disclosures about competitive overlaps, management structures and deal rationale. The FTC argued the changes were necessary to modernize merger review and detect anticompetitive transactions. But the judge ruled that the agency exceeded its authority and did not demonstrate that the rule’s benefits outweighed compliance costs, which could nearly triple the time required to complete filings. The court stayed the rule to allow the FTC to appeal, which it did by yesterday’s deadline.
- The Gist: This remains a headache for hospitals considering a merger. The time and resources saved on paperwork could be redirected toward patient care, as the American Hospital Association has pointed out. As it stands, hospitals exploring a merger face a paperwork burden that could slow or even stop some deals. The case is now pending in the Fifth Circuit Court of Appeals. Hospitals planning transactions need to watch the news; until the dust settles, those needing to file a pre-merger notification form may navigate some uncertainty.
- Amazon expands same-day pharmacy delivery. Amazon last week announced it would expand its same-day pharmacy delivery service to 4,500 cities nationwide. The move expands Amazon’s market share against other drug delivery providers like Walmart and CVS Caremark. It adds same-day delivery services to 2,000 communities, including remote areas in Alaska, the Navajo Nation and islands only accessible by ferry and only navigable by horse-drawn carriage. The expansion demonstrates the retail giant’s ability to scale its logistics network in healthcare, offering faster access to medications compared with traditional mail-order pharmacies, which can take up to 10 days to deliver drugs.
- The Gist: Amazon entered pharmacy delivery in 2018 when it acquired Pillpack. It has since kept growing even as the pharmaceutical industry faces staffing shortages, transportation barriers and an uncertain policy environment. Beyond using its logistics network, Amazon Pharmacy is also expanding into in-person and digital care through its One Medical practices (which feature pharmacy kiosks) and its Prime membership model. The totality gives Amazon a touchpoint at nearly every step of the pharmacy transaction: a patient can join the network to lower drug costs without insurance, see a clinician in person or by telehealth and fill the prescription at a kiosk or have it delivered to their home the same day, almost anywhere. For a recent entrant with just 1% market share, that is a significant reach.
- Younger adults are getting sicker, study finds. The rate of healthcare claims for younger adults is rising at nearly double that of the baby boomer generation, a report released this week from UnitedHealthcare and the Health Action Council found. While patients older than 61 continue to spend more, millennials (ages 29 to 44) and Generation Z (ages 13 to 28) saw the largest spending rate increases from 2023 to 2025. Gen Z’s year-over-year spending jumped 18%, nearly double the growth rate of baby boomers, the report found. The percentage of millennials considered “well” declined as chronic conditions and medical complexity increased. Nearly one‑third lived with a metabolic condition, and 23% had behavioral health needs. The report also found that while virtual care use has declined, younger adults continue to prefer virtual care and comprised 40% of virtual care use as their PCP utilization declined. As patients age out of adolescence and into adulthood, PCP utilization drops, especially for men, and rebounds as they reach 30 to 39 years old.
- The Gist: As the workforce skews younger, healthcare costs are still projected to rise. This counters conventional thinking: healthcare spending has always increased with age, so a younger population should, in theory, cost less. But these data show the opposite: spending is climbing faster among younger people. Rethinking primary care for younger adults will be critical. When fewer patients consistently seeing a PCP, health systems may need to create stronger incentives to establish or maintain those relationships. Healthcare organizations may need to consider better transitions between adolescent and adult primary care and ensure they have the right partners and payer contracts in place to enable coordinated and more appropriate care.
Plus—what we’ve been reading.
- More than a mortgage: the rising cost of health insurance. Published late last month in The Wall Street Journal, this article puts the rising cost of Affordable Care Act premiums into perspective as enhanced premium tax credits, which made insurance more affordable, lapsed Jan. 1. For a growing number of Americans, the price of health insurance now exceeds their monthly mortgage payment. Many households are now seeing premiums double or more, pushing monthly payments past $1,000 for family coverage. In some markets, this exceeds the typical mortgage payment. The result is a jarring reset in household budgets, as families that once viewed marketplace coverage as manageable confront bills that feel more like a second housing payment.
- The Gist: The mortgage comparison is a shock that reshapes how consumers think about the value of coverage. When healthcare insurance starts to compete with housing for a place in the monthly budget, some consumers face uncomfortable decisions as insurance grabs an increasing share of their paychecks. Some are trading down to less generous plans with higher deductibles; others are opting out of insurance altogether. Both scenarios increase the likelihood of delayed care and bad debt for hospitals. This reality pressures volumes on the front end and margins on the back end, particularly in markets with high marketplace enrollment. But the larger risk is cultural: if coverage is perceived as overpriced relative to tangible assets, public tolerance for premium increases and provider price growth may erode quickly. Health systems should expect sharper scrutiny from policymakers and patients who now see the insurance bill in the same mental category as the mortgage.
Graphic of the Week
A key insight illustrated in infographic form.
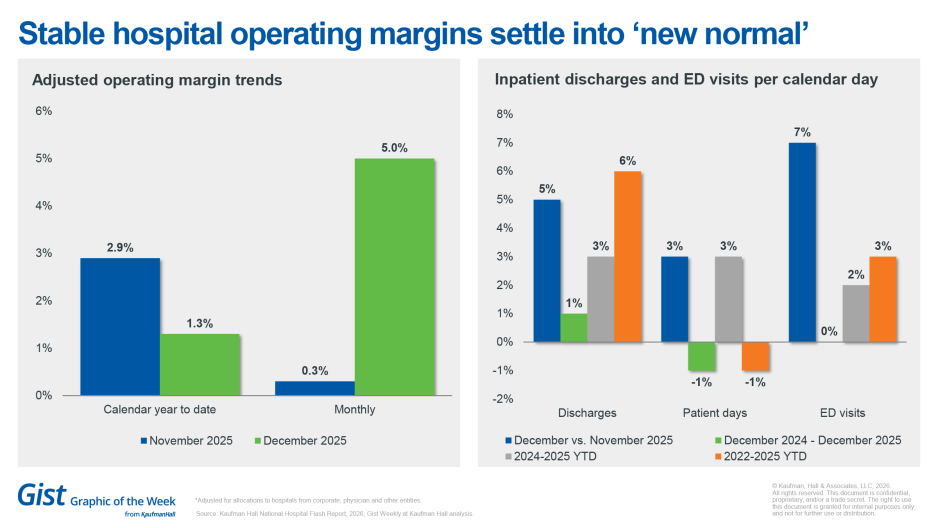
Stable hospital operating margins settle into ‘new normal’
The most recent National Hospital Flash Report highlights stabilizing hospital margins at the end of 2025. Year-to-date margins closed out at a median of 1.3% when adjusted for the allocations to hospitals from corporate, physician and other entities. December also saw month-over-month and year-over-year increases in inpatient discharges, patient days and emergency department visits. With patient volumes moderately rising, hospitals will likely experience a greater demand for high-acuity care with elevated costs. This comes as expenses, particularly bad debt and charity care, rise across the board, suggesting hospitals will need to prepare for this new normal.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
Partnerships don’t fail because of bad intent, but they might fail because of avoidable missteps taken early in the partnership process, often in moments of optimism and goodwill.
In a new article, Andre Maksimow and Nora Kelly examine why well-intentioned partnerships unravel and how to prevent it. Drawing on transaction experience, they highlight five practical lessons, from building a credible business case early to aligning incentives and avoiding overly complex governance structures. These insights offer tangible guidance for leaders seeking to secure partnerships that deliver value to their organizations and the communities they serve.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Last Monday, we began a two-part conversation on the decline of rural family physicians, examining what happens when a community loses its only doctor, from reduced access to care to the broader ripple effects across small towns.
This Monday, host J. Carlisle Larsen concludes the series with Dr. Colleen Fogarty of the University of Rochester, exploring what it will take to rebuild the rural physician workforce, from training pipelines to immigration pathways, and where there are signs of progress.
To stay up to date, be sure to tune in every Monday, Wednesday and Friday morning. Subscribe on Apple, Spotify, Google or wherever podcasts are available.
Thank you for reading! Please stay tuned for next week and check out our Gist Weekly archive for past editions. We also have our recent Graphics of the Week available here.
The Gist Weekly team at Kaufman Hall