In the News
What happened in healthcare recently—and what we think about it.
- Hantavirus outbreak tests U.S. preparedness. U.S. and international health officials this week sought to reassure the public after an outbreak of hantavirus on an international cruise ship led to three deaths and several illnesses. “This is not the next Covid,” an official from the World Health Organization told the Associated Press. Eighteen Americans who were passengers on the cruise ship were evacuated last week to specially equipped quarantine hospitals in Nebraska and Georgia, although only two patients showed symptoms that were reported as mild. Hantavirus is a zoonotic, rodent-borne virus that can cause severe and sometimes fatal lung disease in humans. While the virus is typically not transmissible from human to human, the Andes strain is transmissible—and also has a long incubation period of about six weeks. The cruise ship departed from Argentina April 1, and the first patient who contracted the disease died on board April 11; his wife died two weeks later.
- The Gist: A new outbreak of an infectious, zoonotic disease evokes some unhappy memories. But, while the situation continues to evolve, health authorities insist that the threat level appears to be low. Still, the outbreak raises readiness concerns, especially in the wake of recent funding cuts and the United States’ departure from the World Health Organization. In the short term, hospitals will have a role in reassuring the public as questions come in around the lack of targeted treatments. With memories of the Covid-19 pandemic still uncomfortably fresh, some health systems are preparing; several have built specialized facilities for quarantine and biocontainment. For most hospitals, this is probably an appropriate opportunity to revisit preparedness planning.
- Fair weather for major insurers? Major health insurers reported strong first quarter earnings. Several payers, including UnitedHealthcare, Aetna, Cigna, Elevance Health, Centene, and Alignment Healthcare, upgraded their earnings guidance while Humana, Molina Healthcare, and Clover Health beat their projections. Humana also reaffirmed its adjusted profit forecast but lowered its non-adjusted earnings forecast. Payers attributed their success to premium increases, benefit cuts, exits from unfavorable markets, reduced utilization, and better management of medical costs. Stock prices have risen since January, and the recent Medicare Advantage (MA) rate increase may have also contributed to stronger performance this quarter.
- The Gist: Insurers have struggled for years and appear to be finding their footing. While these results are just a point in time, the first quarter of 2026 has been a welcome reprieve for many payers. While the MA rate increase may have helped their stock prices, their improved operating performance has much to do with more strategic, disciplined portfolio decisions and proactive planning in late 2025. Nevertheless, payers must continue to brave the weather; expiration of Affordable Care Act enhanced tax subsidies, Medicaid funding changes, and continued regulatory uncertainty will keep payers on their toes. Fairer weather for insurers may not mean a reprieve from complex contract negotiations and day-to-day operating challenges—but the roadmap to closer payer-provider collaboration demands the hard work of building trust, aligning incentives, and sharing information.
- Overdose deaths continue to fall, but a new threat is emerging. The United States saw another significant decline in drug overdose deaths in 2025, according to data released this week by the Centers for Disease Control and Prevention (CDC). This marks the third straight year of improvement after the devastating peak of the fentanyl crisis. Preliminary data estimate roughly 70,000 overdose deaths in 2025, down nearly 14% from 2024 levels and far below the more than 110,000 deaths recorded in 2023. Much of the improvement stems from fewer fatalities tied to synthetic opioids such as fentanyl, alongside broader naloxone access, expanded addiction treatment, and greater public awareness of overdose risks. The CDC’s National Vital Statistics System described the trend as a sustained and encouraging reversal after years of record mortality. The news comes as the White House earlier this month released its National Drug Control Strategy.
- The Gist: The data offer reason for optimism. Emergency departments and behavioral health teams are beginning to see the benefits of years of investment in harm reduction, medication-assisted treatment, and community outreach. But experts warn not to get too comfortable. A new family of synthetic opioids known as “orphines” has begun appearing in the U.S. drug supply, with some compounds reportedly many times more potent than fentanyl and difficult to detect with existing test strips. The drugs have been identified in 14 states, primarily in the South and Midwest. Public health officials worry these substances could undermine recent gains, particularly if surveillance, addiction treatment funding, or harm-reduction programs weaken. Despite the good news from the CDC, hospitals can expect continued pressure to expand toxicology capabilities, strengthen overdose-response protocols, and integrate addiction care more directly into acute and ambulatory settings if orphine use becomes widespread.
Plus—what we’ve been reading.
- The Gist: The data offer reason for optimism. Emergency departments and behavioral health teams are beginning to see the benefits of years of investment in harm reduction, medication-assisted treatment, and community outreach. But experts warn not to get too comfortable. A new family of synthetic opioids known as “orphines” has begun appearing in the U.S. drug supply, with some compounds reportedly many times more potent than fentanyl and difficult to detect with existing test strips. The drugs have been identified in 14 states, primarily in the South and Midwest. Public health officials worry these substances could undermine recent gains, particularly if surveillance, addiction treatment funding, or harm-reduction programs weaken. Despite the good news from the CDC, hospitals can expect continued pressure to expand toxicology capabilities, strengthen overdose-response protocols, and integrate addiction care more directly into acute and ambulatory settings if orphine use becomes widespread.
- Newborn vitamin K deficiency deaths on the rise. Published in ProPublica last week, this investigation examines the sharp increase in hospital-reported vitamin K shot refusal, and the resulting rise in vitamin K deficiency bleeding (VKDB), a rare but potentially fatal condition. The investigation reviewed autopsies, hospital records, and federal data showing that some infants who did not receive the injection later suffered catastrophic brain bleeds and seizures, and some died. Babies who do not receive vitamin K are 81 times more likely to develop late VKDB, with roughly 1 in 5 affected infants dying.
- The Gist: Vitamin K is an internationally accepted, safe, and effective newborn intervention. The public, however, appears to be uncertain. Vitamin K administration—which is available via injection and oral drops (which are less effective)—is not routinely tracked by hospitals nor federal level. Nor has vitamin K deficiency bleeding ever been submitted for consideration as a condition clinicians are federally required to report, limiting monitoring. This lack of infrastructure is worsened by poor clinical recognition. Frontline teams have limited experience diagnosing and treating the rare condition. As a result, hospitals are left ringing the alarm, with individual facilities reporting refusal rates as high as 20%. In the absence of federal guidance, hospitals may wish to consider developing internal methods to track administration rates and building competencies around identification, counseling, and emergency care for a condition modern newborn care protocols had largely eliminated.
Graphic of the Week
A key insight illustrated in infographic form.
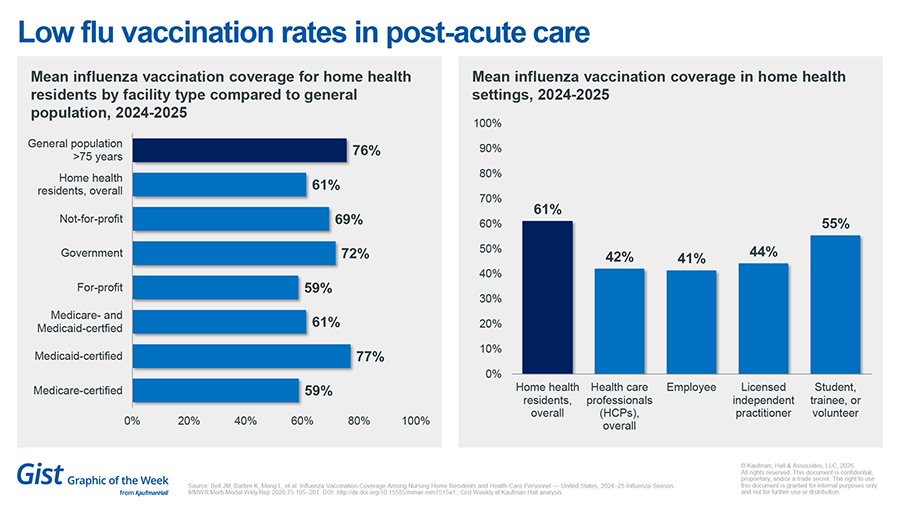
Low flu vaccination rates in post-acute care
Flu vaccination rates are higher for nursing home residents than they are for the healthcare professionals caring for them, the CDC’s latest report indicates. The CDC found that across facility types, nursing home residents were less likely to be vaccinated than similarly aged people in the general population (75.6%). Medicaid-certified facilities were the only exception, with vaccination rates resembling those of the same age. Meanwhile, healthcare professionals caring for residents had even lower vaccination rates (45.4%), although independent practitioners, students, trainees, and volunteers reported comparatively higher rates. Overall, healthcare professionals in nursing home settings were less likely to be vaccinated than those in acute care settings (80.7%), suggesting that targeted education for nursing home staff and their residents may be an important lever for protecting this vulnerable population.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Coming up on Monday, we get the latest healthcare business and policy news, including a look at a new CMS initiative that would streamline prior authorizations.
To stay up to date, be sure to tune in every Monday, Wednesday, and Friday morning. Subscribe on Apple, Spotify, Google, or wherever podcasts are available.
Thanks for reading! The Gist will be on hiatus next week in preparation for the Memorial Day holiday. We will return with a new edition on May 29. In the meantime, check out our Gist Weekly archive for past editions. We also have all our recent Graphics of the Week available here.
Best regards,
The Gist Weekly team at Kaufman Hall