In the News
The biggest news of the week—and what we think about it.
- Maternal mortality lowest since 2018. Maternal mortality rates continue to decline, according to a Centers for Disease Control and Prevention (CDC) report published this week. The report found that maternal mortality has declined from 18.6 deaths per 100,000 live births in 2023 to 17.9 in 2024. Yet the news comes as a new CDC analysis indicates that fewer pregnant patients are receiving prenatal care in their first weeks of pregnancy, risking reversal of the maternal mortality trend. From 2021 to 2024, the CDC found, first-trimester prenatal care initiation dropped 4%, second-trimester initiation rose 12% and initiation in the third trimester or not at all rose 16%.
- The Gist: The U.S. maternal mortality rate remains higher than in most high-income countries, and although mortality declined after the pandemic, this progress is fragile. Nearly 87% of pregnancy-related deaths are preventable, and maternity deserts, insurance coverage gaps and changing patient preferences threaten recent gains. More patients are delaying or skipping prenatal care, even as alternative approaches—such as free-birthing, or childbirth without medical assistance—gain traction. Home births increased 74% from 2021 to 2024, underscoring the growing influence of personal beliefs, care preferences and trust in clinicians on maternity decisions. Hospitals and health systems can meet the moment by strengthening patient education and redesigning prenatal care models to prevent maternal health gains from slipping away.
- Mississippi system suffers major cyberattack. A ransomware attack last week led to the shutdown of all of University of Mississippi Medical Center’s facilities. The system suffered a nine-day shutdown as clinicians turned to manual entry and care continued in an analog environment. All elective procedures were called off as the attack affected many aspects of the enterprise, including the electronic health record, health system officials said. The system worked with the FBI and Homeland Security to handle the attack, which officials said was financially motivated.
- The Gist: Cyberattacks on health systems are profoundly disruptive. They have become increasingly common, making cybersecurity and digital resiliency a necessary investment. Their operational and financial implications are wide-reaching, with cybersecurity and preparedness becoming a critical consideration for disaster management, strategic planning and financial stewardship. Cybersecurity has become a strategic priority, as attacks are a matter of when and how, not if. The salient question is: how are hospitals prepared to respond when the inevitable attack comes?
- Medicare Advantage growth slows. Medicare Advantage (MA) enrollment rose to a record high of 35.4 million in 2026, but the program’s growth rate has slowed, from 3.6% last year to 2.5% this year, an analysis published last week has found. Special needs plans comprise the bulk of new enrollment, data show. The new analysis, which reviewed data from the Centers for Medicare & Medicaid Services from 2022 to 2026, found that seven states saw MA enrollment declines as payers shifted and insurance plan products shrank. The market has changed, as exits from UnitedHealth Group and Aetna made way for Humana’s 21% jump in enrollment and paved the path for increased enrollment in newer plans.
- The Gist: Medicare Advantage is undergoing a marked shift. More than half of the Medicare population is enrolled in Medicare Advantage, even as signs of trouble appear. Major plans are working overtime to control costs and some are looking for a way out as quality and financial pressures mount. But troubles in the MA market do not catch industry leaders by surprise. Almost seven out of 10 MA leaders expect their membership to remain flat or contract by 2027, while they also expect benefits to diminish, the report found. As benefits change, health systems face the prospect of additional administrative burden due to greater use of prior authorization and changing reimbursement.
Plus—what we’ve been reading.
- Drug ads under fire. Published last month in The New York Times, this article describes the renewed push to stop direct-to-consumer prescription drug advertising, a practice allowed only in the United States and New Zealand. Direct-to-consumer advertising dates to 1997, when the Food and Drug Administration (FDA) loosened rules for televised drug promotions. The practice expanded after Medicare Part D was launched in 2006, as research found that ads can shape patient requests and prescribing. But it appears a backlash is forming. A presidential memo last fall urged for restoration of the 1997 restrictions, and the FDA has issued multiple warnings over misleading ads. Last year, a bipartisan bill was introduced in the Senate to put a stop to the practice.
- The Gist: Pharmaceutical companies spent $9 billion on drug ads last year, and more than $200 million on Ozempic alone between 2022 and 2024. Critics say the ads push costly drugs with limited added therapeutic value, while advocates argue they contribute to patient education and surface underdiagnosed conditions. Both can be true; however, it appears drug companies usually spend on advertising before their patents expire and stop advertising once generics are available, suggesting that patient education may not be the priority. The prospects for a full ban are unclear, but policy pressure is creating some support for a three-year moratorium on advertising for newly approved drugs.
Graphic of the Week
A key insight illustrated in infographic form.
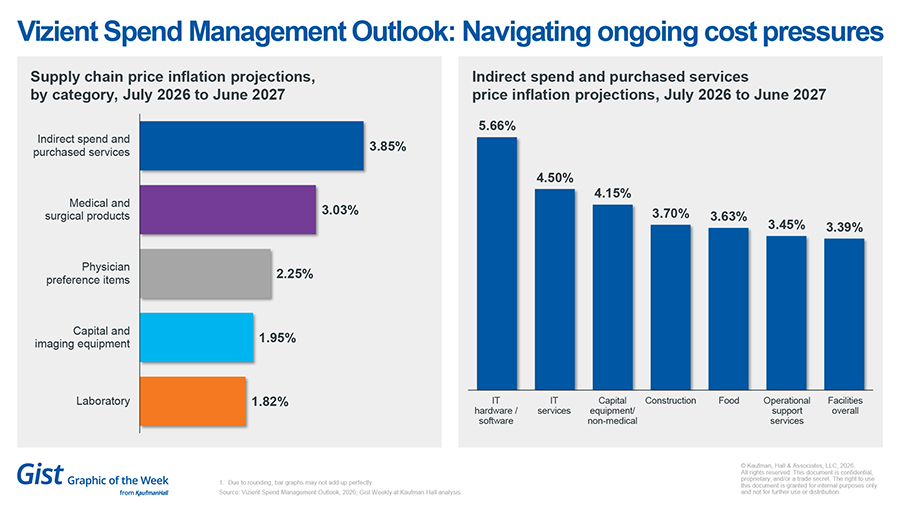
Vizient SMO: Navigating ongoing cost pressures
The latest Vizient Spend Management Outlook projects a 2.78% overall increase in healthcare supply chain prices for July 2026 to June 2027. Pharmacy price growth is projected at 2.84%, but, for the first time in more than a decade, pharmacy is no longer the fastest-growing non-labor expense: IT and facilities-related costs now lead projected inflation, the report finds. This signals a shift in how hospitals must approach budget planning. Agile sourcing strategies and a deep understanding of market risk will be critical for organizations continuing to navigate economic and operational headwinds over the next year.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
Healthcare organizations are continuously looking for funding sources for a wide range of capital needs, including new debt issuance, facility upgrades, technology investments and liquidity enhancements. Both traditional and alternative capitalization strategies can help balance these needs with balance sheet preservation.
A new article explores the current capital outlook for health systems—and how leaders can chart strategies that best meets their organizations’ long-term needs.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Earlier this week, host J. Carlisle Larsen spoke with Kaufman Hall Managing Director Joyjit Choudhury about site-neutral payment and what it means for health system strategy. This Monday, we listen to the conclusion of their conversation in which JC and Joyjit discuss what execution looks like and what cost restructuring may demand as reimbursement shifts.
To stay up to date, be sure to tune in every Monday, Wednesday and Friday morning. Subscribe on Apple, Spotify, Google or wherever podcasts are available.
Thank you for reading! Please stay tuned for next week and check out our Gist Weekly archive for past editions. We also have our recent Graphics of the Week available here.
The Gist Weekly team at Kaufman Hall