In the News
The biggest news of the week—and what we think about it.
- FTC announces new Healthcare Task Force. The Federal Trade Commission (FTC) last week announced the formation of a new Healthcare Task Force, a multibureau effort that it said will “engage in a coordinated, integrated approach to healthcare enforcement.” The task force pulls together staff from the FTC’s competition, consumer protection and economics bureaus, along with its policy planning and technology offices. It is charged with leading targeted investigations, aligning the agency’s investigatory strategy, and identifying new areas for enforcement, including emerging issues in healthcare markets and healthcare technology. The group will also work with other federal departments such as the Departments of Justice and Health and Human Services, the FTC said in its announcement.
- The Gist: In its public announcement, the FTC did not outline specific areas or issues the task force would be considering in its work. One immediate question arises: does this mean more aggressive scrutiny of mergers and acquisitions? The FTC isn’t saying so explicitly. But it is consolidating its internal silos, which could translate into more consistent and potentially closer scrutiny of transactions, pricing practices, and competitive behavior. In its announcement, however, the FTC did trumpet recent actions, including a settlement with Express Scripts and affiliated entities requiring changes to their business practices, and a successful challenge to a proposed device company merger. The announcement raises more questions than it answers, such as: are there particular deals that might be subject to additional investigation? What does this mean for certain sectors of the healthcare field, such as pharmacy benefit managers or AI? Will the FTC look kindly at proposed health system partnerships with physicians? Although it’s too early to tell, the agency’s specific mention that “consolidation and anticompetitive conduct have distorted the economic landscape in many healthcare markets” suggests a renewed focus on market power and consumer impact.
- Moody’s issues negative outlook for insurers. The health insurance sector outlook remains negative, according to a Moody’s Ratings report published last week. Analysts warn that payers face “limited prospects for profitable growth,” largely due to medical inflation, higher utilization and medical complexity, and expensive drugs. In response, insurers are considering plan redesigns, benefit cuts, and leaving underperforming markets, Moody’s analysts said. The report also points to mounting regulatory scrutiny and ongoing enrollment pressures. It said that a return to a stable outlook would require better cost control, more disciplined pricing, and clear gains from value-based care and digital health, but cost pressures remain complex and persistent.
- The Gist: Health systems may be tempted to respond to insurers’ troubles with tiny violins. But temper your enthusiasm: as insurer margins tighten, hospitals will feel the heat. Hospitals need all components of the ecosystem to function well. Payers are likely to respond with moves that will translate into tougher contract negotiations, tighter utilization management, and more frequent prior authorizations and denials. At the same time, reducing benefits raises the risk of more under- and uninsured people, driving uncompensated care and bad debt. To mitigate these pressures, hospitals may explore boosting eligibility verification, financial counseling, financial assistance, and patient navigation programs. They will also likely need to sharpen their value proposition in payer negotiations, leveraging cost and quality data.
- No new measles cases as of last Friday. For the first time in months, a week went by in South Carolina with no new confirmed cases of measles being reported. This keeps the number of cases in the state at 997. If the trend continues for 42 days, or twice the incubation period for measles, South Carolina can declare an end to its measles outbreak, experts said. South Carolina’s Department of Public Health said 93% of its current cases were in unvaccinated individuals.
- The Gist: The end of the nation’s largest measles outbreak may be in sight, which would be welcome news. Even so, measles outbreaks are occurring around the country at a time when patients are increasingly hesitant to vaccinate. The real fear is that measles could be the first of several diseases to reemerge; a further fear is that reemerging infectious diseases may not be as contagious but could be much more dangerous. Cases of Hib and tuberculosis are already popping up. Any break from measles is a rare moment of good news; but health organizations must promote practices to keep these diseases in the past.
Plus—what we’ve been reading.
- A new risk for patients: Dr. AI. Published earlier this month on NPR, this article details how millions of people are now turning to tools like ChatGPT for health information. The results can be unreliable and, in some cases, dangerous; one recent study found that users consulting AI correctly identified a medical condition only about one-third of the time and chose the right next step just 43% of the time. Another concern is inconsistency: small differences in how a patient describes symptoms can lead to very different recommendations, including missing life-threatening conditions. Even when AI identifies the right diagnosis, it may fail to convey urgency, underestimating the severity of emergency situations in more than half of cases. There is research indicating that AI can perform well in controlled settings and even outperform humans, and there are some instances in which experts believe its use is beneficial; but real-world use can be far messier, and many patients lack the training to ask the right questions or interpret responses correctly.
- The Gist: For years, patients have been relying on Dr. Google, often contrary to their medical providers’ advice. AI threatens to make an existing problem worse: it is already shaping patient decision-making, sometimes in clinically inappropriate ways. Patients may arrive having delayed care, misunderstood symptoms, or followed flawed guidance. At the same time, the technology is not going away, which means providers will need to actively guide how it is used. This includes educating patients on AI’s limits, reinforcing the importance of clinical evaluation, and, in some instances, integrating AI into controlled, clinician-led workflows. There is also a broader trust issue at play, as health systems are increasingly expected to differentiate credible medical guidance from algorithmic guesswork. In practical terms, this is about reaffirming the role of clinical judgment in a world in which patients show up with a chatbot in their pocket.
Graphic of the Week
A key insight illustrated in infographic form.
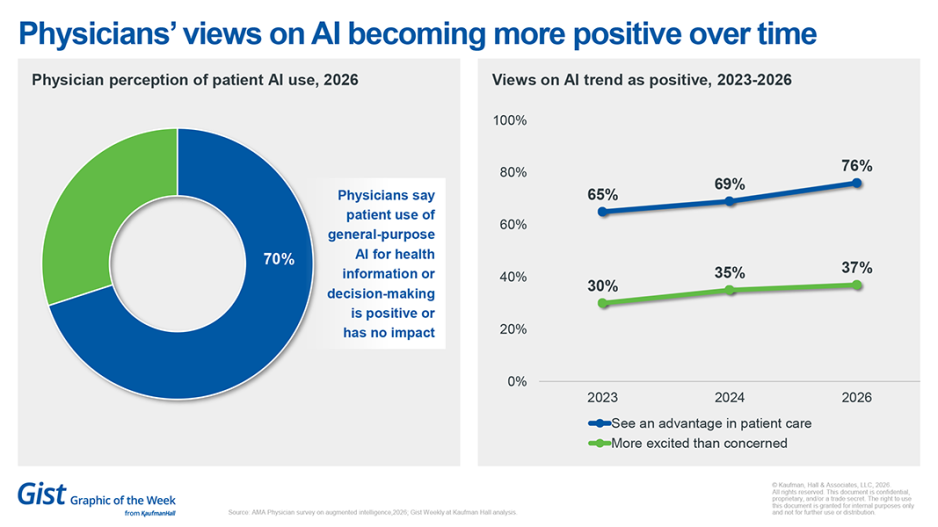
Physicians’ views on AI becoming more positive
The latest physician survey from the American Medical Association (AMA) indicates physicians’ views of AI are turning more positive over time. Comfort with and use of AI has grown, according to the AMA, which found that 80% of physicians now use AI professionally. The survey found that more than 76% of physicians believe AI can help their ability to care for patients, up from 65% in 2023. It also found that 70% of physicians believe that patients’ use of general-purpose AI chatbots for health information or decision-making is positive or has no impact. While doctors express concerns over patient privacy (86%), relationship-building, and skill loss (88%), they also believe that more training and inclusion of physicians in AI development (85%) will help over time.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
Academic medical centers’ traditional funding model, built on hospital margins subsidizing research and education, is breaking down under pressure from rising costs, workforce shortages and weakening reimbursement. This creates a growing structural imbalance that threatens the mission.
This new article argues that sustainability now depends less on how much organizations spend and more on tighter governance, alignment, and accountability to ensure resources are used strategically across the enterprise.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Earlier this week, host J. Carlisle Larsen spoke with Phil Englert of Health-ISAC about the recent cyberattack on Stryker, an unusual and disruptive incident that didn’t follow the typical ransomware playbook, and what it reveals about how these threats are evolving.
Coming up Monday, JC continues the conversation with Englert, looking at how healthcare organizations respond in real time, what the incident reveals about medical device safety, and how the industry coordinates when systems are under pressure.
To stay up to date, be sure to tune in every Monday, Wednesday, and Friday morning. Subscribe on Apple, Spotify, Google or wherever podcasts are available.
Thank you for reading! Please stay tuned for next week and check out our Gist Weekly archive for past editions. We also have our recent Graphics of the Week available here.
The Gist Weekly team at Kaufman Hall