In the News
The biggest news of the week—and what we think about it.
- Cyberattack strikes Stryker. The medical device manufacturer Stryker’s internal Microsoft environment was compromised late last week in a cyberattack that experts attributed to the Iran war, the company announced. The hack affected order processing, manufacturing, and shipping but did not jeopardize any of its products, the company said. Experts said the attack did not result in direct impacts or disruptions to U.S. hospitals using Stryker products. Organizations that order through distributors will experience a typical ordering experience, but new client organizations ordering directly through Stryker may experience a delay, the company said.
- The Gist: The healthcare field continues to be a target for hackers. The attack comes on the heels of a warning from the cybersecurity monitoring advisory group Health Information Sharing and Analysis Center, which warned U.S. health organizations earlier in March of the potential for cyberattacks as retaliation for U.S. military strikes on Iran. This incident is a direct attack on the U.S. healthcare community. Stryker says that the attack has been contained, but the potential for harm and disruption across the healthcare community and its products is a wake-up call. Cybersecurity is increasingly top of mind for hospital executives, and is magnified by greater geopolitical uncertainty.
- Insurer pays up. Aetna, a major Medicare Advantage (MA) insurer, has agreed to pay $117.7 million for submitting and failing to withdraw inaccurate codes for its MA enrollee claims, the Justice Department (DOJ) reported this week. DOJ alleged that Aetna sought to increase its Medicare payments, with its allegations centering on chart reviews that add diagnosis codes that medical records support but were never made by a physician. These additional diagnoses inflate risk adjustments and payments made to the plans, DOJ said. The settlement is expected to resolve the charges.
- The Gist: This is not the first instance of a settlement for inappropriate coding for MA plans. The Medicare Payment Advisory Commission has found that MA plans cost Medicare more than traditional Medicare, and congressional investigations have found that patients have overpaid premiums because of Medicare overpayments. This settlement appears to be part of a crackdown on Medicare overbilling, especially by insurers with MA plans. For health system executives with long memories, the settlement may be reminiscent of the late 1990s and early 2000s, when the Justice Department aggressively pursued cases against healthcare organizations.
- Court blocks HHS vaccine schedule changes. A federal judge on Monday temporarily blocked the Trump administration’s overhaul of the childhood vaccine schedule, halting a series of changes pushed by Health and Human Services Secretary Robert F. Kennedy Jr. The preliminary injunction invalidates recent actions taken by a newly appointed federal vaccine advisory panel after Kennedy dismissed all 17 prior members last summer, a move the court said likely violated federal law and established procedures. It also suspends a revised immunization schedule that reduced the number of recommended childhood vaccines and eliminated broad guidance for several diseases, including flu and hepatitis. The decision came in response to a lawsuit from major medical groups, including the American Academy of Pediatrics (AAP), which argued the changes were made without scientific review or proper process. The court’s order freezes both the policy changes and the advisory committee’s recent votes. Federal officials have indicated they will appeal, setting up a legal fight that could ultimately reach the Supreme Court.
- The Gist: The ruling restores a measure of short-term clarity but does not resolve the underlying instability. Federal vaccine guidance drives clinical protocols, payer coverage and pharmacy operations, and the past several months have introduced confusion about what standards to follow. Many states and health systems have already defaulted to recommendations from groups like the AAP, and this decision effectively reinforces that workaround for now. The larger issue is governance: when federal processes are disrupted, hospitals, clinicians and patients are forced to navigate conflicting guidance, complicating care delivery. There is also a financial dimension, since vaccine recommendations are closely tied to reimbursement and supply chain planning. Continued uncertainty around national vaccine policy is to be expected until the legal questions are settled.
Plus—what we’ve been reading.
- Trust can cure vaccine hesitancy. Published last week by The New York Times, this article tells the story of a Kentucky mother who lost trust in the medical system after a challenging hospital experience with her infant daughter, where, she said, clinicians dismissed her questions and threatened her. She found support in a community that encouraged her questions and recommended skipping vaccines. The article describes an environment in which clinicians face a landscape shaped by abundant misinformation and diminished trust in their expertise. For this mother, returning to traditional care and catching up with vaccinations began not with data, but with a trusting patient-clinician relationship. She turned to a pediatric nurse practitioner who remained patient, nonjudgmental, and open to answering questions, creating a ripe condition for the patient to reengage.
- The Gist: Building and maintaining a trusting relationship with patients may be one of the few levers providers have to restore patients’ trust in vaccines. Patients still overwhelmingly trust their doctors, and training is evolving to match—teaching clinicians to be less judgmental and more patient. But this requires time, which is always in short supply. It’s even more challenging in inpatient and emergency settings, where patients usually meet clinicians often for the first time in a hectic environment. There, clinicians are more likely to suffer the consequences of misinformation, shifting a burden on to the hospital. Creating space for patient-provider relationships to help earn patient trust may be just what the doctor ordered.
Graphic of the Week
A key insight illustrated in infographic form.
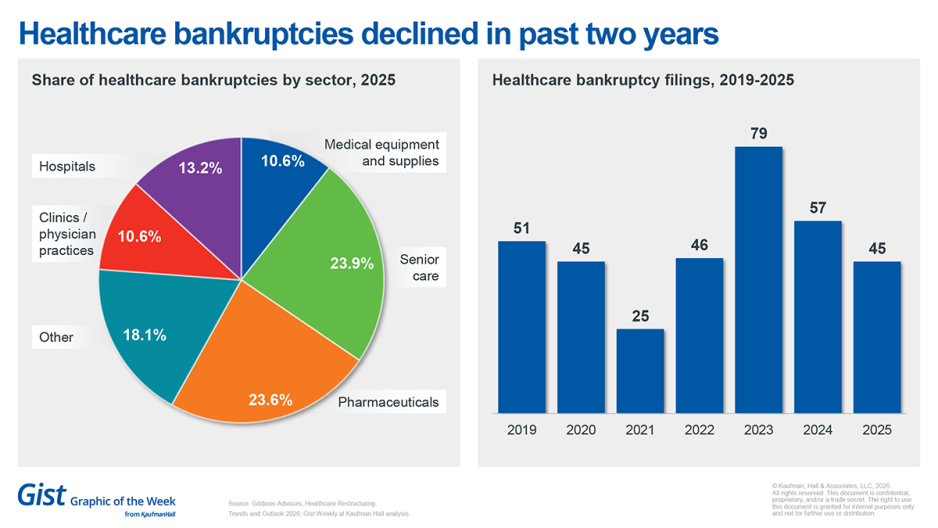
Healthcare bankruptcies declined again in 2025
Healthcare bankruptcy filings decreased for a second consecutive year, according to a recent report from Gibbons Advisors. The report finds a 21% decline in bankruptcy filings year-over-year, with the bulk of the 45 filings in 2025 occurring in the first quarter. The bankruptcy activity appears to be tempering, adjusting to pre-pandemic trends. By sector, senior care and pharmaceuticals comprise about half of the bankruptcies, with hospitals only accounting for 13.6% of all healthcare bankruptcy filings in 2025.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
Join us March 25 for the Kaufman Hall Rating Agency Spring 2026 Update, a live, complimentary webinar featuring leaders from Moody’s, S&P and Fitch as they discuss the latest industry outlooks, rating activity through early 2026, and what it means for the not-for-profit healthcare sector.
Moderated by Kaufman Hall’s Robert Turner and Lisa Goldstein, the webinar will cover topics including evolving federal policies, capital planning amid reimbursement changes, how AI strategies factor into bond ratings, the heightened threat of cyberattacks coming from the Iran conflict, and perspectives on non-traditional financing structures. Learn more and register today!
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Earlier this week, host J. Carlisle Larsen spoke with Michael McAuliff of Moder Healthcare to get the latest in how healthcare policy is shaping up on Capitol Hill, and how healthcare could play a role in the upcoming midterm election.
Coming up Monday, the cyberattack on the medical device manufacturer Stryker stood out as an unusual and highly disruptive incident that quickly raised concerns across the healthcare field. JC speaks with Phil Englert of Health-ISAC about the incident and what it means for the field.
To stay up to date, be sure to tune in every Monday, Wednesday, and Friday morning. Subscribe on Apple, Spotify, Google or wherever podcasts are available.
Thank you for reading! Please stay tuned for next week and check out our Gist Weekly archive for past editions. We also have our recent Graphics of the Week available here.
The Gist Weekly team at Kaufman Hall