In the News
The biggest news of the week—and what we think about it.
- Measles cases spread; will other infectious diseases follow? Utah this month confirmed 300 measles cases in an ongoing outbreak, with the virus now spreading in Salt Lake County and new exposures at high schools in that county. The new outbreak comes as the South Carolina measles outbreak this week showed encouraging signs of abating, with lower numbers of new cases reported for the second consecutive week. A growing number of measles cases were reported in Georgia, Ohio and Florida in February as well. Federal officials this month reported seven new outbreaks in 2026, with a total of nearly 1,000 confirmed cases nationwide. Meanwhile, the Maryland Department of Health this month confirmed an increase in mumps cases in the state.
- The Gist: Measles is highly contagious and, before a vaccine was introduced in 1963, caused 2.6 million deaths per year. Its spread is likely abetted by lower vaccination rates and by sporadic public reporting requirements. But its resurgence may portend something worse. Some experts consider it the canary in the coal mine, signifying that other, even more serious infectious diseases (such as pertussis, meningitis or even polio) may be around the corner. Clinicians and provider organizations nationwide should be dusting off their playbooks for how to recognize and treat measles and other infectious diseases previously thought to be consigned to history books.
- Major healthcare strikes wind down. New York City’s largest nurses strike in decades concluded last weekend after 41 days, with the final holdouts ratifying new three-year contracts that include raises, staffing protections, workplace violence safeguards and other terms. Nurses at NewYork-Presbyterian/Columbia University Medical Center joined peers from Montefiore Medical Center and Mount Sinai Health System in voting yes and began returning to work late last week. The strike involved roughly 15,000 nurses and followed months of stalled negotiations. Meanwhile, an estimated 31,000 Kaiser Permanente registered nurses and other healthcare workers in California and Hawaii ended a four-week strike Tuesday, even with no new contract in place, after what union leaders described as progress at the bargaining table. They returned to their jobs this week.
- The Gist: Both labor actions drew widespread attention to workforce shortages and workers’ discontent. Hospitals coming off prolonged strikes are left holding a complex set of realities. Staff have secured meaningful contractual gains, but some workers may still harbor resentment, which can erode morale and foster distrust. At the same time, hospitals operated under intense cost pressures well before the strikes, and rising costs of supplies labor and benefits now eat into already thin margins. Balancing competitive wages and staffing levels with financial sustainability will continue to strain budgets, leaving executives to manage hostility among staff and financial stress from payers.
- CBO projects Medicare trust fund will be exhausted by 2040. The Medicare Hospital Insurance Trust Fund (Part A) will run out of money in 2040 under current law, significantly earlier than previous projections, according to a Congressional Budget Office (CBO) update published Monday. According to the CBO analysis, the trust fund’s balance will grow through 2031, but then spending will exceed revenue until reserves are depleted in 2040. The change reflects weaker revenue projections from payroll taxes and higher expected Medicare spending per enrollee, including inpatient hospital care and related services. This revised insolvency date is roughly 12 years sooner than the CBO’s 2025 projection. The CBO’s findings come as other long-term budget pressures challenge Medicare, as the population ages and per-person costs rise.
- The Gist: CBO’s projection does vary from year to year, and 2040 is a long time from now. Additionally, it varies significantly from the more relied-upon projection by the Medicare Trustees, who typically issue their report in June. Nevertheless, hospitals should take this projection seriously, even if the forecast shifts with future estimates. Part A Medicare reimbursements largely fund hospital inpatient care but also cover some skilled nursing and hospice care and insolvency could threaten those reimbursements. The projection underscores the importance of continuing to engage with federal policy on Medicare financing and new payment models. Even with uncertainty around the exact exhaustion date, the direction of long-term financing pressures calls for strategic planning around revenue diversification, efficiency and risk management. Hospitals should consider trust fund projections a risk factor in multi-year financial planning rather than a fixed deadline.
And—and what we’re following.
- The family of Henrietta Lacks, the Baltimore woman whose cells were extracted for medical research without her consent 75 years ago, has settled a lawsuit with Novartis.
- New reports from the Centers for Disease Control and Prevention indicate U.S. childhood and teen obesity rates have reached record highs while adult obesity rates may be slowing.
Plus—what we’ve been reading.
- Price transparency efforts eclipse patient needs. Published earlier this month in KFF Health News, this article examines renewed federal efforts to require hospitals and insurers to publicly post their prices. While the policy was intended to address surprise billing and empower consumers, compliance has been uneven, and the data, when available, are often buried in hard-to-interpret spreadsheets. There is little evidence that patients use the information to compare prices, and medical care is rarely standardized enough to shop like retail goods. Instead, the primary users of the transparency data are hospitals and insurers, who rely on competitors’ posted rates in contract negotiations. What was envisioned as a consumer-focused cost-control tool has become merely a lever in industry pricing battles, with scant evidence that it lowers costs for patients.
- The Gist: Price transparency was meant to empower patients as informed consumers. Instead, it is apparent that the power of transparency is limited without standardization. Spreadsheets filled with billing codes may technically satisfy requirements but do little to help patients understand what they may owe. Critics say only a fraction of hospitals comply with the law and assert that compliance has become the ceiling, not the floor. If transparency becomes a regulatory box to check rather than an opportunity to innovate around clear, standardized, understandable pricing, the data will never serve the public. The risk: price transparency may become just another expensive paperwork exercise that does little to help patients.
Graphic of the Week
A key insight illustrated in infographic form.
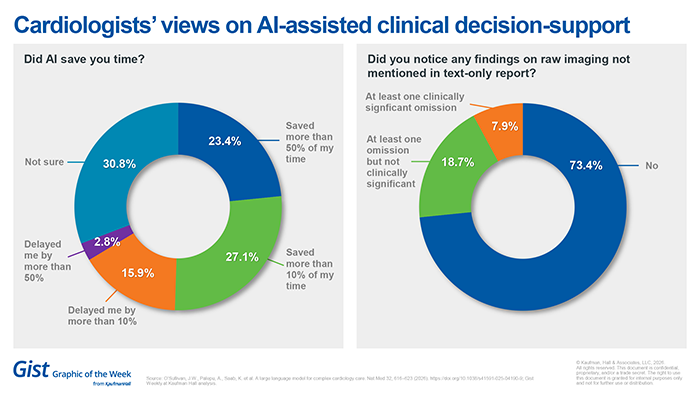
Cardiologists’ views on AI-assisted clinical decision support
New research published this month in Nature explores the role of AI in clinical decision support. Researchers asked cardiologists about perceived time savings, efficiency, hallucinations and omissions. They found that cardiologists found clinically significant omissions in nearly 8% of cases. Yet they also found that cardiologists working without AI assistance had more clinically significant errors than those assisted by AI. Cardiologists also report that AI helped their assessment more than half the time and saved time in at least half of their cases. The study gets to the issue of confidence in the technology: if clinicians trust AI tools, they can save time and improve care despite staffing shortages.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
Healthcare leaders often ask what the “right” level of investment in AI-enabled solutions is for their organization—but they may be asking the wrong question.
A new article explores why the financial sustainability of AI adoption efforts may depend less on how much organizations spend—and more on whether those investments move through a disciplined, structured capital allocation process.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
Earlier this week, we heard the conclusion of host J. Carlisle Larsen’s two-part conversation with Colleen Fogarty, M.D., of the University of Rochester, about the declining numbers of family physicians in rural communities.
This Monday, site-neutral payment is shifting from policy debate to operational reality. In a two-part conversation, Kaufman Hall Managing Director Joyjit Choudhury explains how health systems can assess their exposure and what cost restructuring may demand.
To stay up to date, be sure to tune in every Monday, Wednesday and Friday morning. Subscribe on Apple, Spotify, Google or wherever podcasts are available.
Thank you for reading! Please stay tuned for next week and check out our Gist Weekly archive for past editions. We also have our recent Graphics of the Week available here.
The Gist Weekly team at Kaufman Hall