In the News
What happened in healthcare recently—and what we think about it.
- Mandatory bundled payment may be around the corner. The Centers for Medicare & Medicaid Services (CMS) has proposed mandating a nationwide bundled payment model for joint replacements—with some exceptions. In its FY2027 Inpatient Prospective Payment System and Long-Term Care Hospital Prospective Payment System proposed rule published April 10, CMS proposed a new model, Comprehensive Care for Joint Replacement Expanded (CJR-X). CJR-X would require most hospitals (again, with some exceptions) to take financial accountability for hip, knee, and ankle replacements and their follow-up care. The proposed rule also contains an increase in hospital payment rates by 2.4%, which CMS estimates would add roughly $1.4 billion in total payments. Public comments are due June 9, with a final rule expected later in 2026 ahead of an Oct. 1 implementation.
- The Gist: CMS’s focus on value-based care gained momentum in 2010, when Congress created the Center for Medicare and Medicaid Innovation under the Affordable Care Act. Early efforts included the Comprehensive Care for Joint Replacement (CJR) Model, which ran from 2016 through 2024. The proposed expansion into CJR-X demonstrates that CMS leaders are eager to build on the original model’s results around both savings and quality of care. Joint replacement, as one of the most common inpatient procedures, serves as a high-impact test case for a standardized approach to bundled care delivery and payment. But, if finalized, CJR-X would require some hospitals to change the way they do business. Its mandatory nature is sure to cause consternation among some hospitals that don’t want to make the switch.
- Teen births decline to record low. Teen births fell by 7% from 2024 to 2025, according to data published last week. The latest data, from the Centers for Disease Control and Prevention’s (CDC’s) National Center for Health Statistics, finds that the fertility rate for 15- to 17-year-olds declined by 11% from 2024 to 2025, while the rate for 18- and 19-year-olds fell by 7%. These were both record lows, the CDC said. The overall fertility rate declined by 1% for women of reproductive age and is down 23% since 2007. While births to women under 30 have declined, births to women 30 to 35 have remained flat and births to women of “advanced maternal age” (age 35 and older) have increased. The report also found that preterm birth rates remained unchanged while Cesarean delivery increased to 32.5% from 32.4% in 2024, the highest since 2013. The low-risk Cesarean delivery rate rose to 26.9% from 26.3%, the highest since 2012.
- The Gist: While the overall fertility rate decline has been a cause for concern for some time, the decline of teen births is a major public health victory. Changing fertility rates point to a demographic shift, with more women possibly delaying childbearing as they pursue careers. Hospitals with obstetric service lines should prepare for a continued increase in high-risk pregnancies that are associated with advanced maternal age. This may pose additional challenges for obstetrics units in rural settings that may see increasing complexity and even less volume.
And—what we’re following.
- A new Medscape report finds physician compensation rose by about 3% in 2025.
- A federal judge dismissed a lawsuit filed by an Elevance Health subsidiary alleging that HaloMD and several providers coordinated to exploit the No Surprises Act’s dispute resolution process.
- CMS selected 150 digital health companies and providers to launch ACCESS, a 10-year payment model that reimburses technology used in chronic care management based on patient outcomes.
Plus—what we’ve been reading.
- AI-assisted medical bill disputes. Published last week in The New York Times, this article describes how patients are increasingly using AI chatbots to interpret and challenge medical bills—often with incomplete understanding and mixed results. It describes how, as healthcare cost concerns rise, patients turn to AI to navigate complex billing statements, identify potential errors, and draft appeals. In one case, a Washington, D.C., couple used a GPT to contest a $22,604 emergency department bill. The chatbot produced a letter with flawed legal reasoning. (The bill was ultimately waived.) In another instance, a chatbot failed to identify the correct regulatory pathway for an insurance dispute; in a third, it buried mention of financial assistance programs that ultimately led to a bill being forgiven.
- The Gist: Patient engagement and financial literacy are unequivocally positive endeavors. As affordability concerns continue, the use of AI to help patients understand their care and take charge of their medical bills is a natural progression. Yet chatbots, while helpful in translating jargon and suggesting next steps, often provide incomplete or misdirected advice. These uneven results are not only frustrating to navigate for hospitals and patients; they expose growing gaps in health and financial literacy that are further widened by the digital divide. Getting ahead of a potential influx of AI-generated disputes will likely mean that hospitals need to step in early and support financial literacy and navigation.
Graphic of the Week
A key insight illustrated in infographic form.
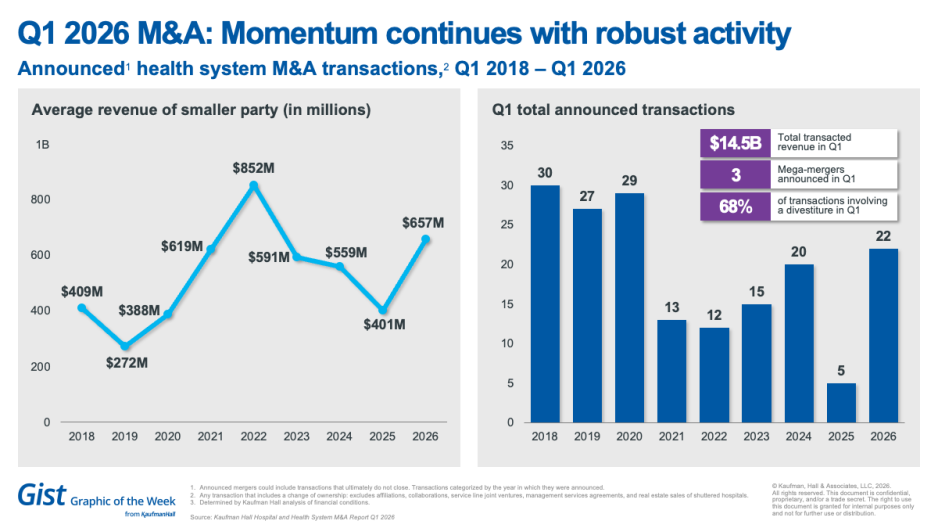
M&A momentum continues with robust Q1 activity
Hospital and health system M&A activity continued with momentum in the first quarter of 2026, with 22 hospital and health system transactions announced—the highest first-quarter activity since 2020, according to the Kaufman Hall Mergers and Acquisitions Q1 Report. Activity this quarter continues a steady recovery in M&A activity that began in the second half of 2025. With three “mega-mergers” among the 22 announced transactions, deal size rebounded. The average size of the smaller party increased, and total transacted revenue reached $14.5 billion—a recent high.
This Week at Kaufman Hall
What our experts are saying about key issues in healthcare.
After several years of elevated downgrade pressure, rating agencies are reporting growing stabilization for hospital ratings.
Kaufman Hall’s recent 2026 Spring Rating Agency Update highlights key insights from leaders at Fitch Ratings, Moody’s Ratings and S&P Global Ratings on upgrade/downgrade trends and the overall hospital sector outlook.
On Our Podcast
The Gist Healthcare Podcast—all the headlines in healthcare policy, business and more, in 10 minutes or less every other weekday morning.
JC spoke with Robert Wachter, MD, Chair of the Department of Medicine at the University of California, San Francisco and author of A Giant Leap: How AI Is Transforming Healthcare and What That Means for Our Future, about what feels different in this current wave of AI in healthcare—and what lessons from the rollout of electronic health records still apply.
This Monday, the conversation continues with a closer look at one of the first real use cases: AI scribes. Dr. Wachter and JC discuss why scribes have been adopted so quickly, how they’re changing clinical workflows, and what they reveal about how this technology is taking hold in practice.
To stay up to date, be sure to tune in every Monday, Wednesday, and Friday morning. Subscribe on Apple, Spotify, Google, or wherever podcasts are available.
Thanks for reading! We’ll see you next Friday with a new edition. In the meantime, check out our Gist Weekly archive for past editions. We also have all our recent Graphics of the Week available here.
Best regards,
The Gist Weekly team at Kaufman Hall