
This is the second article in a three-part Performance Improvement Series. The final article will explore strategies for engaging physicians in performance improvement.
Hospital and health system leaders have historically focused their cost reduction initiatives on streamlining or improving how the organization’s resources are deployed, from labor to supplies to facilities. But an opportunity to save millions of dollars by reducing length of stay is hiding in plain sight every time a patient walks through the front door.
Emerging care management approaches are focused on coordinating each step in a patient’s care journey, from tracking status at admission, to anticipating and avoiding denials, to coordinating with community-based providers after patients are discharged. Care management teams can also help staff members improve how they document and track key milestones throughout the episode of care.
Adopting a team-based approach to care management can be challenging. Frontline staff may lack the training to appropriately track and assign patient status from the different portals of entry, which may complicate discharge planning. A lack of communication between financial and clinical departments can result in knowledge gaps regarding contract requirements, and lead to costly denials. Convincing physicians to work on reducing length of stay can be difficult without actionable data that links improvements in the quality of patient care with financial goals.
Carefully executed care management initiatives that start with staff training, and ultimately manage the entire episode of care across the continuum, can address discharge “bottlenecks,” reduce length of stay, and make major contributions to organization-wide performance improvement efforts. In some instances, the resulting reductions in length of stay might open up enough capacity to delay the construction of new additions or even new facilities.
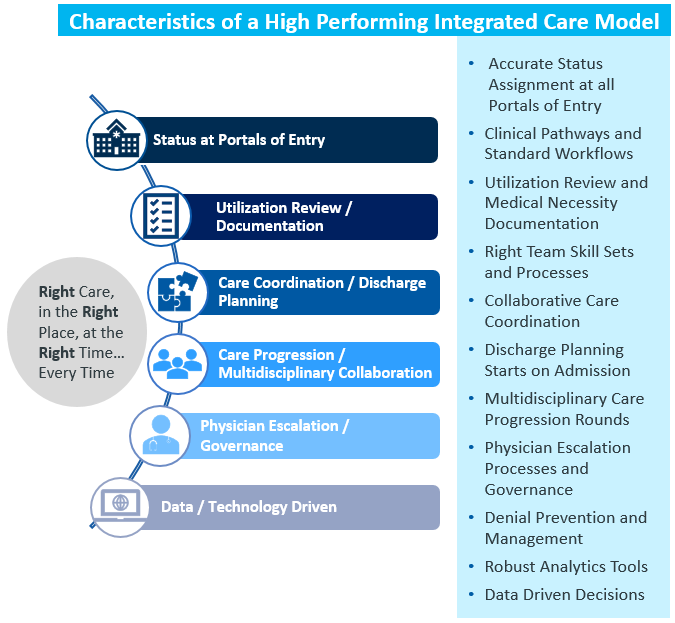
Forging an Integrated, Data-Driven Approach
Only 14% of hospital leaders who responded to the Kaufman Hall/HFMA 2019 Healthcare Performance Improvement survey said their clinicians would say they have access to actionable information to address clinical variation. In turn, only 4% of respondents reported success reducing variation, and 25% of respondents named it as the area of greatest difficulty.
Emerging analytics that integrate cost and quality data can help hospitals identify opportunities to reduce length of stay, using Medicare’s Geometric Mean Length of Stay (GMLOS) as a baseline. An integrated approach can also be used to foster greater organizational collaboration. Care management teams that effectively engage business leaders, hospitalists, post-acute partners, and other clinical leaders in reviewing data and determining potential solutions can forge a more consistent approach for managing everything from medical necessity documentation to ensuring discharge criteria are uniformly applied.
Care Management Across the Continuum
At the outset of care management initiatives, relevant hospital employees should be trained to understand and fulfill patient precertification and regulatory requirements. Care management teams must also ensure that every portal of entry to the facility uses a consistent process for tracking patient status from the moment they arrive. Once a patient is admitted, the care management team can initiate planning for discharge, and ensure that any throughput barriers are addressed in real-time.
The care management team should also work closely with emergency department physicians and hospitalists to track the status of patients, ensure the collection of needed documentation for medical necessity, and help prevent unanticipated denials.
Hospitalists and other physicians also play a critical role. Daily multidisciplinary rounds for each patient can help ensure clinicians collaboratively identify a discharge plan, medical milestones, and throughput barriers, and help address potential bottlenecks hours before they occur.
Successful care management teams continue their work after discharge. By collaborating with physician practices, insurers, and community-based providers, care management teams can help support efforts to keep patients healthier in their communities and avoid costly readmissions.
Setting Targets for Reducing Length of Stay
Using the tactics described above, one hospital located in the Northeast with approximately 400 beds, had an opportunity in 2019 to make significant improvements in length of stay.
By subtracting the number of inpatient days an organization expected in a fiscal year based on the Medicare GMLOS from the observed or actual number of inpatient days in that same fiscal year, hospitals can determine their excess day opportunity. The organization uncovered a potential opportunity between roughly 1,600-5,000 “excess days” in one calendar year.
At an average cost of roughly $640 in savings with each excess day, the potential savings opportunity is between approximately $1 million and $3.2 million. In 2020, the hospital’s leaders intend to employ the interventions outlined in this article to eliminate remaining excess days.
This represents significant cost-reduction and revenue-improvement progress, even at the lower end of improvement achievement. Organizations with leading care management practices in place typically can achieve a 35-40% reduction in excess days, through targeted and facility-specific interventions.







